Clinical Case Example
Hemimandibular reconstruction with bipedicled free vascularized fibula flap and 3D printed patient-specific plate
Challenge
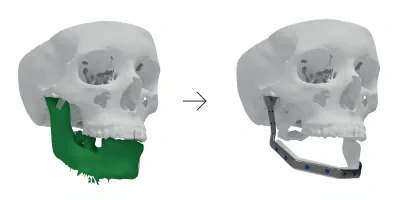
An elderly male patient was diagnosed with a benign tumor in the mandible. Computed tomography demonstrated an expanding lesion in the right path of his mandible. The patient needed a radical removal of the tumour followed by hemimandibular reconstruction.
To achieve optimal functional and esthetic results, reconstructive surgeons had to restore not only the skeletal buttresses and bilateral symmetry, but also the internal soft tissue envelope, and provide a foundation for dental rehabilitation.
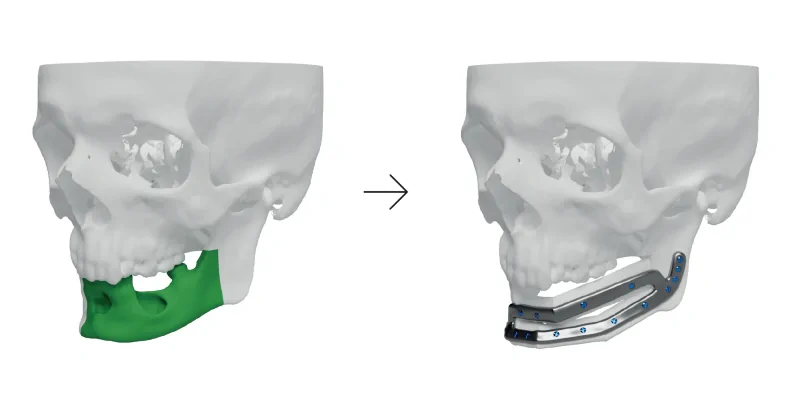
Solution
Surgeons decided to reconstruct the defect using the fibular graft. However, using a single fibula bone for mandibular reconstruction may produce a height discrepancy between the native mandible and the grafted fibula that results in subsequent difficulty in wearing conventional dentures or osteointegrated implants. To circumvent this problem, surgeons decided to use double-barrel free vascularized fibula.
Accurate resection and precise arrangement of bone grafts are necessary to obtain a good result in multi-graft reconstructions cases. Using the Customy 3D Planner during the preoperative planning, the surgeon can view the virtual 3D patient’s anatomy and all designed for him patient-specific products. What’s more, the surgeon can interact with the 3D patient’s model and define cutting planes for lesion resection.
Based on the surgeon’s guidelines and having defined the cutting planes for tumor resection, our engineer planned mandibular reconstruction using four-elements fibula graft. The next step was to design the surgical cutting guides (one for the tumor resection and one for harvesting fibula grafts) adjusted to the surgical instruments. Finally, the custom plate was designed according to the patient’s anatomy. The reconstruction plan with all patient-specific products was presented in the Customy 3D Planner for the surgeon’s approval.
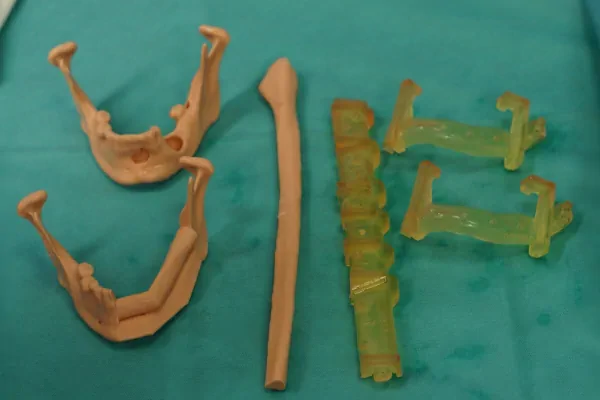
The Customy RecoBox contained the titanium patient-specific double-barrel reconstruction plate, two surgical cutting guides and anatomical models of patient’s mandible (before and after surgery).
Surgery
The first part of the surgery focused on the resection of the lesion and surrounding tissues using the patient-specific surgical cutting guide. Then the vascularized fibula bone graft was harvested using the second surgical guide. Grafts with skin islands were used in the reconstruction of a composite defect from a tumor and positioned according to the preoperative plan. The microvascular anastomosis was performed to supply grafts with blood. Bone grafts were stabilized by patient-specific plate and fixed by screws. To finish procedure soft tissues around mandible were restored.
Results
Using patient-specific products like surgical guides allowed surgeons to accurately transfer the surgical plan to OR. The original mandibular contour was maintained by a custom-made plate. Microvascular fibula transfer was completely successful, and all skin paddles survived without necrosis. The face functions in the short term results were very good.
The 3D preoperative planning helped to minimize complications and allowed surgeons to carefully think through the procedure.